Reiki Training and Resilience in Oncology Nurses:
A Mixed Methods Study
Summary: This COMIRB-approved study was conducted in 2021-2022 at the UCHealth Anschutz Cancer Center. Fifteen oncology nurses participated in this four-month Reiki training program, and notable improvements in resilience were recorded.
- Principal Investigator – Lynne Bentley, PhD, RN, AOCNS
- Wendy Haylett, PhD, RN, UCHealth Research Department
- Sandy Priester, MBA, CHTP, RMT, LifeSpark Cancer Resources
Background / Purpose
- Oncology nurses are burning out and leaving the profession in large numbers. Increasing nurse resilience is one way to address this problem.
- Resilience in nurses leads to improved patient outcomes because they are more likely to exhibit presence, focus, and compassion in their care for others.
- Self-Reiki practice can reduce stress and anxiety and promote a sense of well-being. This could increase resilience and lower burnout.
- A prior pilot in 2020 with five Anschutz Cancer Center (Aurora, Colorado) nurses revealed a 17% increase in resilience scores upon completion of First and Second Degree Reiki training.
As a result of the pilot study mentioned above, our team developed a second research study, conducted in 2021-2022. Its purpose was to evaluate the impact of Reiki training and Self-Reiki practice on a larger number of oncology nurses. It was COMIRB-approved and included additional longitudinal measurements and a control group for real-time comparison.
Participants
All who participated in the study were oncology nurses working at the UCHealth Anschutz Cancer Center with 80% working in an out-patient cancer unit. 93% were female, all had at least a 4-year degree, and 67% had been an oncology nurse for at least 5 years. All were non-Hispanic white, 86% were either married or in a partnership, and their ages spanned the 20s through the 50s. 80% had experienced energy work in the past.
Methods
Design of the Study
This was a mixed methods study with a semi-crossover and repeated measures design.
- Nurses were randomly assigned to Cohort 1 (n=6) or Cohort 2 (n=9).
- Cohort 1 was initially trained in Reiki, while Cohort 2 was the control. Once Cohort 1 was trained, Cohort 2 received the same training.
- The Connor-Davidson Resilience Scale (CD-RISC) and investigator-developed qualitative questions were used to evaluate resilience.
- Surveys were administered before the training, at its conclusion, and three-month and six-month intervals thereafter.
Structure of teaching
The training spanned four months to accommodate busy schedules.
- The training covered First & Second Degree Reiki with the following:
- Weekly online content (approximately 2 hours per week)
- Four in-person meetings for attunements and practice sessions
- An expectation of daily 20-minute self-Reiki practice.
Results
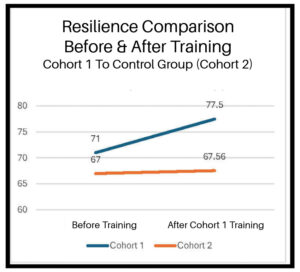 Notable improvements in resilience were recorded for Cohort 1 compared to Cohort 2 (the control group) over the same time period. Cohort one’s average resilience, as recorded by the 110-point CD-RISC, increased from 71 before training to 77.5 after training. Whereas the control group’s resilience went from 67 to 67.5 during this four-month period.
Notable improvements in resilience were recorded for Cohort 1 compared to Cohort 2 (the control group) over the same time period. Cohort one’s average resilience, as recorded by the 110-point CD-RISC, increased from 71 before training to 77.5 after training. Whereas the control group’s resilience went from 67 to 67.5 during this four-month period.
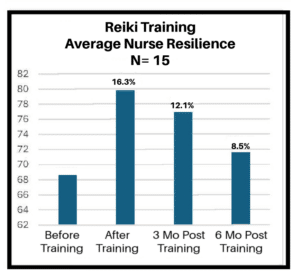 Once Cohort 1’s training was complete, Cohort 2 was then trained, and resilience scores were recorded similarly (before training, at the end of training, and at three- and six-month intervals after training). When combining the results for the two groups, there were notable improvements in resilience between baseline before the training and at the intervals recorded. According to the CD RISC, resilience had improved 16.3% right after training, 12.15% at three months, and 8.5% at the 6-month interval.
Once Cohort 1’s training was complete, Cohort 2 was then trained, and resilience scores were recorded similarly (before training, at the end of training, and at three- and six-month intervals after training). When combining the results for the two groups, there were notable improvements in resilience between baseline before the training and at the intervals recorded. According to the CD RISC, resilience had improved 16.3% right after training, 12.15% at three months, and 8.5% at the 6-month interval.
By the six-month mark, the number of nurses filling out the questionnaires for the study dropped from 15 to 9. Based on their comments, about half likely continued regular or intermittent Reiki practice. However, at least three were no longer practicing, and it was unclear if two others were still using Reiki regularly. This may have impacted the declining resilience scores over time.
Responses to Qualitative Questions
Common themes related to current stressors: Fear of the unknown, lack of control, inability to meet self-expectations, and compassion fatigue.
“I feel I am increasingly disengaged and not as compassionate as I used to be, and that makes me really, really sad.”
Common themes related to the Reiki training and regular self-Reiki practice: Being more reflective, and calm. The need for more external structure to support the practice.
- “Helping me to slow down and continue to set good boundaries.”
- “Decreased feelings of burnout- refill my cup outside of work so that I can endure work without feeling completely drained when I get home.”
- “I am not doing it on a regular basis … I think the structure of being in the study helped keep me more on track.“
Conclusions / Implications
- This study suggests that Reiki training and self-Reiki practice may enhance emotional resilience for oncology nurses handling multiple stressors and experiencing burnout.
- Based on the above results, we suggest that regular self-Reiki practice may be necessary to sustain resilience over time.
- Institutional support and regular gatherings for self-Reiki practice may increase the number of nurses who continue to use this tool.
Next Steps
- Launch a research study with an adequately powered sample size (60+ nurses) to:
-
- further study whether Reiki has a statistically significant impact on resilience in oncology nurses and
- study the impact of daily self-Reiki on the maintenance of resilience over time.
-
- Work with UCHealth to develop structures that support daily self-Reiki practice.
